Women—Your Health Matters!
Perimenopause and menopause present significant challenges for women with migraine, primarily due to dramatic hormonal fluctuations that can trigger or worsen attacks. The instability of estrogen and progesterone levels during perimenopause often leads to unpredictable and more severe migraine attacks, especially for women who already experience menstrual migraine.
Diagnosis becomes complicated as symptoms such as hot flashes, sleep disturbances, and mood changes overlap with both migraine and the menopausal transition itself. Additionally, reliable treatment can be elusive, as hormone replacement therapies or other interventions may not work uniformly or could even make symptoms worse.
A proactive, personalized approach to care is key to preventing migraine progression and reducing its disruptive effects on women's quality of life.
Many thanks to Dr. Natbony for her help with this project and answers to questions.

Watch this video with Dr. Natbony as she discusses how perimenopause and menopause can impact migraine
Watch Our Videos & Read the Blog
Women, do not to give up hope. Remember that migraine is treatable—even though the path can be challenging. No one should feel they have to simply “settle” for persistent symptoms as an inevitable part of aging or menopause.
"Your experiences and symptoms are real and valid. Seeking personalized care, exploring all available treatment options, and believing in the possibility of improvement are essential steps to living better with migraine at any stage of life."
—Dr. Natbony
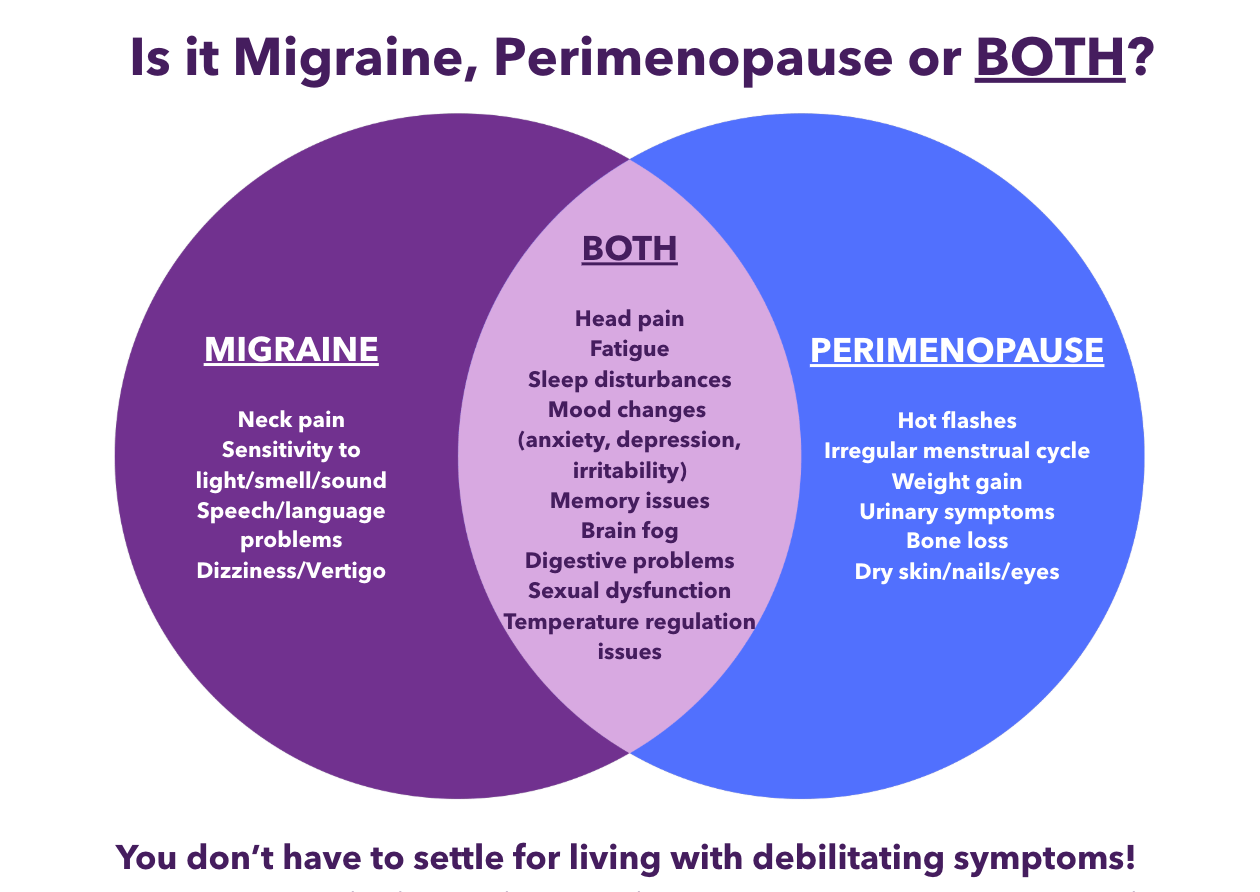
Is it Migraine, Perimenopause or BOTH?
Bring this to your next doctor's appointment and ask your doctor to help you build a personalized plan for managing your migraine during perimenopause and menopause.

Migraine in Perimenopause and Menopause
General Questions
Diagnosis and Treatment
Life Impact and Lifestyle Modifications
About the Doctor
 Lauren R. Natbony, MD, FAHS, is the Founder & Medical Director of Integrative Headache Medicine of New York. She is also an Assistant Clinical Professor of Neurology in the Division of Headache and Facial Pain at Mount Sinai’s Icahn School of Medicine. Dr. Natbony, who suffers from migraine herself, previously served as the Director of the Headache Medicine Fellowship at Mount Sinai and continues to be actively involved in teaching headache fellows and neurology residents. She is board-certified in Neurology by the American Board of Psychiatry and Neurology and in Headache Medicine by the United Council of Neurologic Subspecialties. CLICK HERE to learn more about Dr. Natbony and her medical practice!
Lauren R. Natbony, MD, FAHS, is the Founder & Medical Director of Integrative Headache Medicine of New York. She is also an Assistant Clinical Professor of Neurology in the Division of Headache and Facial Pain at Mount Sinai’s Icahn School of Medicine. Dr. Natbony, who suffers from migraine herself, previously served as the Director of the Headache Medicine Fellowship at Mount Sinai and continues to be actively involved in teaching headache fellows and neurology residents. She is board-certified in Neurology by the American Board of Psychiatry and Neurology and in Headache Medicine by the United Council of Neurologic Subspecialties. CLICK HERE to learn more about Dr. Natbony and her medical practice!
This educational project was made possible in part by a generous donation from: